The Canadian Medical Directives for Specialists (CanMEDS) revision project, due to approach completion in 2026, has identified limitations in the current framework’s ability to address the diverse needs of the Canadian population.
Presented here is a dynamic model — a transformed physician competency framework— that centres inclusive compassion and shared humanity and encompasses mechanisms to actively address existing systemic inequities in health care systems.
The model expands medical expertise and supports physicians to take an action-oriented stance and commit to equity, justice, and addressing health disparities, emphasizing the vital competencies that are required in both physician training and patient care to transform health systems.
The Canadian Medical Directives for Specialists (CanMEDS) revision project is at a crucial juncture, with implications for the medical profession in Canada. Expert groups have identified limitations in the current framework’s ability to address the diverse needs of the Canadian population, raising questions about its adaptability to concepts such as antiracism, social justice, artificial intelligence, and planetary health. Previously, we underscored the imperative to include antiracism as a foundational competency in any reimagining of CanMEDS,1,2 recognizing its pivotal role in combating health disparities. As the CanMEDS revision approaches completion in 2026, it presents a unique opportunity for transformative change in medical practice, informed by anti-oppression, cultural safety, and social justice principles. This prompts a critical examination of whether the existing framework can effectively integrate these vital competencies or if a comprehensive reimagining is necessary. The revision offers an unprecedented opportunity to envision a physician competency framework that not only facilitates, but propels transformative change within health care systems.
Transformative change in medical education and practice2,3 demands explicit integration of anti-oppressive competencies. This shift aims to redefine the physician’s role, moving from a neutral to an action-oriented stance committed to equity, justice, and addressing health disparities. Aligned with the needed transformation of the CanMEDS framework,4 this integration emphasizes the vital competencies required in both physician training and patient care, reflecting the need to combat systemic health care inequities. Progress hinges on cultivating a critical mass of physicians committed to this change, thus paving the way for more equitable and just health care.5
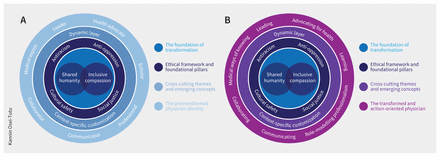
Globally, health care systems grapple with deep-rooted health disparities perpetuated by injustice and biases.6–10 This demands that the physician’s responsibilities extend beyond medical expertise — which is the cornerstone of the profession, as it should be — to encompass principles of inclusive compassion and social justice, adapting to the evolving needs of society. Acknowledging the daunting and challenging nature of transformation, bold visions are needed to catalyze change. I present a vision for the way forward, outlining its potential implications and future directions. This vision places inclusive compassion and shared humanity at the heart of transformative health care (Figure 1A).
(A) A reimagined physician competency model in transformation. Shared humanity and inclusive compassion form its core, cradled by social justice and embraced by its foundational pillars. The “dynamic layer” elevates the sophistication of the model, empowering the integration of crosscutting themes and emerging concepts into a customizable framework that can be tailored to various local and global training and practice contexts. (B) The transformed and action-oriented physician competency model. The “medical expert” role, a cornerstone, is enhanced and expanded to include the latest medical and technological advances, as well as diverse forms of medical knowledge. Each role is transformed from its neutral orientation to its action-oriented stance — drawing inspiration from the model’s core and signalling a commitment to continuous growth and development in all domains across training and practice.
Within this reconceptualized CanMEDS framework, a distinctive competency model emerges, placing inclusive compassion and shared humanity at its core. Symbolized by 2 interconnected circles, these are the foundational principles underpinning the framework. Inclusive compassion underscores the importance of comprehending and addressing the diverse needs of patients, considering their social identities, cultural contexts, and lived experiences, and extending compassion to all individuals without discrimination. Shared humanity recognizes the interconnectedness, intrinsic worth, and dignity that should be acknowledged and upheld for all people regardless of background or identity. The interlocking circles of inclusive compassion and shared humanity represent “intersectionality,” acknowledging the complex and intertwined forms of oppression that affect people across various dimensions such as race, religion, gender, class, socioeconomic status, sexual orientation, ability, and other social identities.11,12 Systemic discrimination cannot be understood or addressed in isolation — the whole person must be seen. By adopting an intersectional lens, this model expects physicians to recognize and challenge the ways in which various forms of oppression contribute to health inequities and strive for more inclusive care. All people ought to be treated as equal in dignity, but not all people are treated equally. The core of the model, deeply rooted in humanistic values, endeavours to reconcile this divide.
Beyond its core, this model seeks to actively dismantle systemic inequities and biases, recognizing their detrimental effects on health care outcomes. Three concentric layers embrace the core and represent the dynamic evolution of values, knowledge, and skills required to redefine excellence in health care. The first layer, closest to the core, encompasses the foundational pillars of antiracism, anti-oppression, cultural safety, and social justice. Antiracism forms a key pillar, as it challenges the perpetuation of racist structures and practices within health care systems.1,13,14 It must be a foundational competency. Anti-oppression recognizes and addresses how power structures and institutional biases can lead to the perpetuation of various forms of oppression. Cultural safety considers the impact of culture on health care experiences15 and social justice advocates for fairness and equal access.16 These pillars provide the ethical framework that can support health care practices free from all forms of bias, discrimination, and systemic injustice, including but not limited to racism, antisemitism, anti-Muslim bigotry, 2SLGBTQIA+ prejudice, sexism, and ableism. By addressing the social determinants of health and advocating for equitable care, physicians can mitigate health disparities and enhance patient outcomes. See Appendix 1, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.231273/tab-related-content, for a glossary of relevant terms.
The next layer, known as the “dynamic layer,” integrates crosscutting themes and emerging concepts into a customizable framework that can be tailored to various local and global training and practice contexts. This layer is characterized by its unique capacity for context-specific customization. It can empower physicians to tailor emerging themes and competencies to the nuanced needs and dynamics of diverse health care environments and practice settings. For example, artificial intelligence (AI), digital health technology, health equity, and planetary health are issues that could fall within the “dynamic layer.” The model invites reflection on the significance of technological literacy when it comes to emerging technologies like AI. Although it holds promise for improving patient care, AI also presents inherent risks, sometimes diverging from the noble pursuit of shared humanity and inclusive compassion.17,18 Positioned at the forefront of innovation, the “dynamic layer” possesses the capacity to integrate the latest advancements and critical considerations essential for modern medical practice. This strategic design ensures the model’s relevance and applicability across a broad spectrum of health care systems and geographical settings, empowering physicians to respond competently to evolving community needs. With its unique capacity for flexibility and customization, the “dynamic layer” not only elevates the sophistication of the model but also enhances its versatility far beyond the confines of the current static CanMEDS framework.
The outer layer represents the transformed and action-oriented physician identity emerging as a direct consequence of the model’s core values and foundational pillars. It signifies a shift in how physicians perceive and embrace their roles and responsibilities within health care. Committed to action, physicians can serve as a catalyst for transformative change within health systems. The model acknowledges the existence of a world characterized by diverse and sometimes conflicting values — tensions exist between traditional healing practices and Western medicine in some communities. Addressing this divide, the model advocates for a nuanced approach to medical expertise, integrating a broader spectrum of systems and perspectives. This inclusive approach mirrors “two-eyed seeing,”19 reflecting a balanced consideration of diverse viewpoints and knowledge systems central to nurturing a more inclusive and compassionate health care environment. Beyond enriching and expanding the traditional “medical expert” role, the model recognizes the crucial importance of medical expertise in defining the physician’s distinctive contribution to health care, while attributing equal value to all component parts of the physician’s identity. This paradigm shift emphasizes the fluidity, integration, and harmony desired from medical experts who navigate multiple roles simultaneously. Lastly, the model strives to inspire an action-oriented physician identity by shifting from static roles to active ones, encouraging physicians to continually evolve and serve as active agents of change within their clinical environments, health care systems, and broader society (Figure 1B).
This model has transformative potential in medical education and health systems. It aligns core values with an action-oriented approach to address social determinants of health and biases. The model integrates social justice principles into medical education, training, and practice, laying a foundation for promoting health equity and improving patient outcomes. The adoption of this model necessitates collective efforts from medical institutions, policy-makers, regulatory bodies, and health care professionals. Crucial next steps include curricula updates, integration of crosscutting themes in professional development programs, mindset shifts, and the provision of additional training and resources.
Beyond individual practice, the model’s implications extend to communities and health systems, empowering physicians as effective leaders in creating inclusive and equitable health care environments. They can challenge barriers, advocate for policy changes, and foster collaborations to drive societal impact and dismantle disparities. To make the model more accessible, future efforts will focus on offering illustrative examples and demonstrating its practical implementation. Subsequent iterations might prioritize streamlining the framework for easier comprehension and implementation. Future directions might involve research and evaluation to determine the model’s effectiveness, as well as exploring interdisciplinary collaboration to address systemic barriers.
This transformed physician competency model promotes the urgent need for equitable health care and champions innovation. By envisioning physicians as agents of change, the model proposed herein challenges the status quo, redefining excellence in health care to align with principles of justice, patient-centred care, and societal impact. Successful implementation and refinement of this model will require collaborative efforts. Together, we can lead transformative change toward a more equitable and compassionate health care system.
Acknowledgements
The author acknowledges Amanda Fisher, graphic designer, Cumming School of Medicine, University of Calgary, for her production of the models; Dr. Nancy Fowler for inspiring the first half of this commentary’s title; and his colleagues in the Canadian Medical Directives for Specialists (CanMEDS) Antiracism Expert Working Group (and others) for their constructive feedback on the first iteration of the model and the suggestion to represent the static CanMEDS roles in their active form.
Footnotes
Competing interests: Kannin Osei-Tutu reports receiving honoraria as a member of the Canadian Medical Directives for Specialists (CanMEDS) steering committee. He is also cochair of the CanMEDS Antiracism Expert Working Group, member of the CanMEDS Professional Role Expert Working Group, and board member of the Black Health Education Collaborative. Dr. Osei-Tutu has also received honoraria as a strategic advisor to the Chief Executive Officer of the Royal College of Physicians and Surgeons of Canada, and support from the Cumming School of Medicine for meetings or travel. Dr. Osei-Tutu has participated on the CanMEDS National Advisory Board.
This article has been peer reviewed.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/